
Many NREMT candidates find themselves staring at questions that feel impossible. A patient with shortness of breath is also pale, sweating, and complaining of chest pain, leaving you unsure whether the scenario is cardiac, respiratory, or shock-related.
The key to cutting through this complexity is identifying Nature of Illness (NOI) clues. These subtle hints are embedded in the patient’s presentation and the scenario details, guiding you toward the correct pathophysiological interpretation and, ultimately, the right answer. Recognizing these clues allows you to quickly prioritize interventions, determine criticality, and confidently choose the next step, even when the question initially feels overwhelming.
NOI clues work because they highlight the underlying problem rather than distract you with minor details. By focusing on these signals, you stop overthinking and start reasoning like a high-performing EMT. The challenge lies in knowing what to look for and how to act on it.
Recognizing Key NOI Patterns
1. Position and Posture Indicators
Patients often communicate distress through their posture. Careful observation can turn a confusing scenario into a straightforward assessment.
- Tripod Position:A patient leaning forward, hands on knees, or hunched over signals severe respiratory distress. This posture is commonly associated with asthma or COPD exacerbations and indicates that immediate attention to airway, breathing support, and oxygenation is required.
- Sitting Upright with Pillows (Orthopnea):When a patient cannot lie flat and relies on pillows to breathe comfortably, this usually points toward fluid overload conditions like congestive heart failure or pulmonary edema. Recognizing this allows you to focus on oxygen delivery, proper positioning, and monitoring for signs of pulmonary compromise.
- Guarding or Fetal Position:Patients curling up or protecting their abdomen often signal acute abdominal emergencies such as appendicitis, peritonitis, or internal bleeding. The posture itself becomes a major clue in narrowing down the correct intervention or transport priority.
2. Respiratory and Airway Clues
Respiratory presentations are common on the NREMT, and NOI hints make them manageable.
- Wheezing:Wheezing, whether inspiratory or expiratory, usually indicates lower airway obstruction, as seen in asthma, COPD, or bronchospasm. When combined with tripod positioning or accessory muscle use, this clue directs attention toward airway support and bronchodilator therapy.
- Crackles or Rales:Crackling sounds during lung auscultation point toward alveolar fluid accumulation, commonly in pulmonary edema or pneumonia. Recognizing this clue prevents misclassification of the patient as purely bronchospastic and ensures proper oxygenation and monitoring are prioritized.
- Slow Breathing with Altered Mental Status:A patient who is shallow-breathing and unresponsive suggests central nervous system depression, often from opioid overdose or sedative effects. The NOI clue here directs immediate airway management and assisted ventilation before other interventions.
3. Cardiac and Vascular NOI Clues
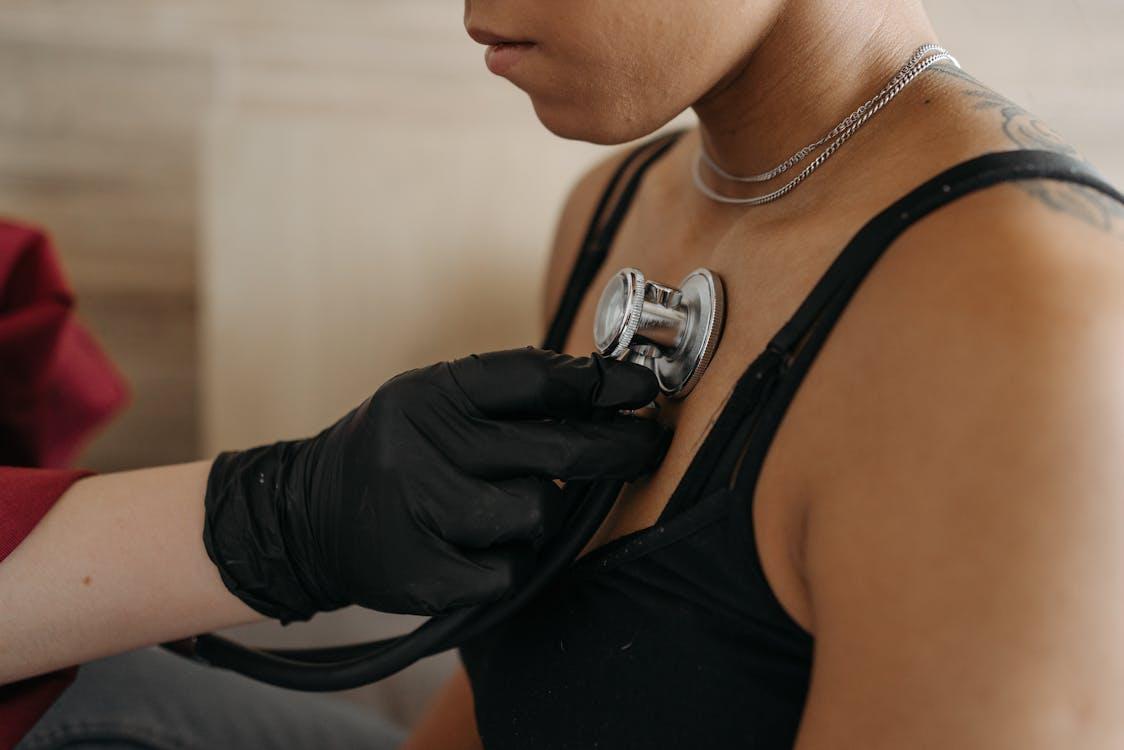
Chest pain and cardiovascular symptoms can feel intimidating, but NOI hints make the answer more obvious.
- Crushing or Pressure Chest Pain with Radiation:Pain described as tightness, heaviness, or radiating to the jaw or left arm signals acute myocardial infarction. Recognizing this clue immediately guides oxygen support, aspirin administration per protocol, rapid transport, and vigilant monitoring.
- Sharp Pain with Breathing:Pain that worsens with inhalation often indicates pulmonary involvement, such as pulmonary embolism, pneumothorax, or pleuritis. This directs your attention to oxygenation, ventilation, and rapid assessment of circulation.
- Increased Pulse with Pale, Cool, Moist Skin:These indicators point toward hypoperfusion or shock. The NOI clue prioritizes circulation support, fluid resuscitation if protocol allows, and rapid transport over other non-critical interventions.
4. Neurological and Metabolic Clues
Subtle neurological hints often indicate underlying metabolic or cerebrovascular emergencies.
- Sudden One-Sided Weakness or Facial Droop:These classic stroke indicators signal a cerebrovascular accident (CVA) and guide urgent transport and rapid evaluation of airway, breathing, and circulation in the proper order.
- Altered Mental Status with Sweating and Clammy Skin:This combination suggests hypoglycemia. Immediate glucose assessment or administration per protocol is indicated, highlighting the NOI clue’s power in identifying the first critical intervention.
- Altered Mental Status with Warm, Dry Skin:Gradual onset with fruity breath often points to hyperglycemia or diabetic ketoacidosis. This distinguishes the scenario from hypoglycemia, ensuring correct prioritization of assessment and monitoring interventions.
5. Environmental and Infectious Clues
Clues often appear in the context of exposure or infection.
- Fever with Productive Cough:Green or brown sputum combined with fever often signals pneumonia. Recognizing this helps you focus on oxygen support, infection monitoring, and identifying signs of respiratory compromise.
- Hives, Swelling, and Airway Involvement:Sudden-onset itching, facial swelling, and respiratory distress suggest anaphylaxis. The NOI clues indicate the need for epinephrine administration per protocol, airway monitoring, and rapid transport, emphasizing time-critical decision-making.
How to Apply NOI Clues Effectively
The real skill lies not in memorizing every possible clue but in applying them strategically during the exam.
- Read the Last Sentence First:Identify exactly what the question is asking (diagnosis, next intervention, or priority assessment) before getting lost in scenario details. This guides which NOI clues are relevant.
- Highlight Key Words:Look for high-yield terms such as “tripod,” “wheezing,” “sudden onset,” or “clammy skin.” These often contain all the information needed to narrow answer choices.
- Evaluate Criticality:Ask which aspect of the patient’s condition poses the most immediate threat. Prioritizing airway, breathing, circulation, or mental status helps eliminate answers that do not address the immediate danger.
- Eliminate and Decide:Remove options that are outside your scope or conflict with the NOI clues. With fewer choices, your odds of selecting the correct intervention improve dramatically.
Using a Combined Strategy

When multiple NOI clues appear in the same scenario, weigh them against the question’s focus.
For example:
- Crushing Chest Pain + Diaphoretic + Pale Skin:Cardiac emergency is more likely than simple anxiety. Prioritize oxygen, monitoring, and rapid transport.
- Tripod + Wheezing + Accessory Muscle Use:Respiratory compromise takes precedence. Focus on airway support and bronchodilator intervention rather than other minor details.
- Altered Mental Status + Fruity Breath + Warm, Dry Skin:Metabolic emergency (DKA) supersedes minor trauma complaints. Assess glucose, airway, and transport priorities first.
By combining posture, respiratory, cardiovascular, neurological, and environmental clues, you begin to form a clear picture from the chaos of multi-system scenarios.
Turning Complexity into Confidence
The NREMT exam’s goal is to simulate real-life ambiguity, but NOI clues are the anchors that allow candidates to remain confident. Recognizing them reduces overthinking, minimizes second-guessing, and keeps the candidate focused on the patient’s immediate needs.
Every confusing scenario can be broken down by observing the subtle indicators embedded in the text. When you rely on these clues rather than trying to memorize every potential detail, questions that once seemed impossible become manageable and even predictable.
About the Author
This blog was written by a clinical education specialist at How To NREMT. They support EMT and paramedic students by providing scenario-based learning, realistic exam simulations, and structured study strategies that develop strong clinical judgment.
How To NREMT offers targeted NREMT exam prep resources to help students identify key patient cues, apply NREMT knowledge effectively, and navigate the cognitive exam with confidence.
Explore their full-access membership and private tutoring options.
FAQs
- How does NREMT scoring work?
The exam uses computer-adaptive scoring. Correctly identifying NOI clues helps maintain consistency on early questions, which influences the difficulty of subsequent items and ultimately impacts your overall score.
- How long should I study for the NREMT exam?
Consistent, scenario-based practice for several weeks is ideal. Emphasizing NOI clues in your study sessions ensures you can quickly extract critical information from each scenario, improving both speed and accuracy under exam conditions.
- How can I pass the NREMT exam?
Passing requires mastering both clinical knowledge and reasoning. Learning to decode NOI clues (like unusual postures, abnormal respirations, or environmental factors) can turn confusing scenarios into clear, actionable steps that increase your chance of success.
- What kind of questions are on the NREMT exam?
Questions often present multi-system patients with overlapping symptoms. NOI clues help you determine whether the priority is respiratory, cardiac, neurological, or metabolic, which guides your choice of correct intervention.






